Conical vs Flat-to-Flat Connection: 5 Differences That Actually Matter
Leggi in Italiano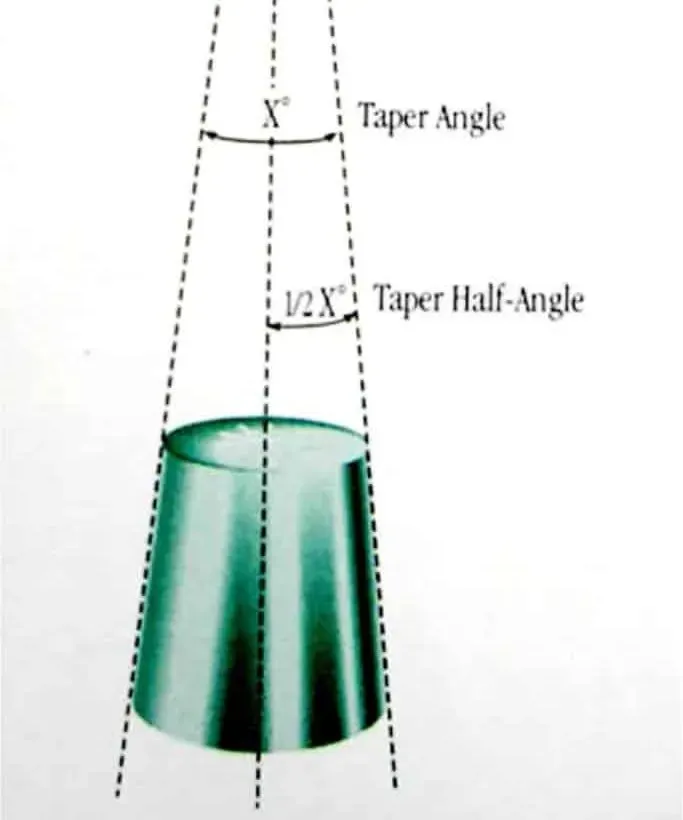
In brief — Conical connections (Morse taper) in dental implants drastically reduce microgaps compared to traditional designs, improving sealing and mechanical stability. Masticatory load progressively increases connection retention. Challenges remain: residual microgaps (1–3 micrometers), cyclic fatigue wear, sensitivity to manufacturing precision, and abutment retrieval difficulty for maintenance.
Sintesi (IT) — Le connessioni coniche (cono Morse) negli impianti riducono drasticamente i microgap rispetto ai design tradizionali, migliorando sigillatura e stabilità meccanica. Il carico masticatorio aumenta progressivamente la ritenzione della connessione. Tuttavia, rimangono sfide: microgap residui (1–3 micrometri), usura sotto carico ciclico, sensibilità alla precisione manifatturiera, e difficoltà di rimozione dell’abutment per manutenzione.
What are the many advantages — and the few drawbacks — of conical connections in implants?
The Evolution of Implant-Abutment Connections
Implant technology has advanced considerably over the past few decades. Among the most promising innovations is the conical connection, born from the Morse taper — designed by Stephen Morse in 1864 to quickly and securely attach milling components to mechanical lathes.
The original Morse taper was very narrow: 5° total, 2.5° per side. In dental and orthopedic applications (hip prostheses), the angle can be and often is wider.
This design represents a natural evolution over traditional flat-to-flat connections. It offers a more sophisticated biomechanical approach to the challenge of long-term implant-prosthetic stability. As seen when analyzing implant macrogeometry and primary stability, every design detail significantly influences clinical performance.

The conical connection is built on an established engineering principle: the taper coupling creates a retention system that progressively gains stability under load.
In our specific case, masticatory load increases connection stability. This mechanism is already widely used in other industrial sectors. In implantology it finds a particularly advantageous application, where interface stability is critical for treatment success.
And the mechanism actually works.
When we unscrew abutments with a conical connection, the screws are invariably loose — despite having been properly torqued at placement. It is clear that masticatory load increases the intimate engagement between the connection surfaces. This is directly related to what happens at the blood-titanium interface in the critical early moments of integration.
Documented Clinical Advantages
Scientific research has extensively demonstrated the benefits of conical connections through in vitro, in vivo, and clinical studies. The results are convincing and clinically meaningful.
One of the most significant advantages is the ability to drastically reduce microgap formation at the implant-abutment interface.
This is fundamental for long-term success. Microgaps represent a preferential pathway for bacterial infiltration, which can lead to serious complications including mucositis, peri-implantitis, and marginal bone loss (Schmitt et al., 2014; Carnovale et al., 2020; Riberti et al., 2025; Vinhas et al., 2020).
Superior mechanical stability is another well-documented strength. Studies have shown that conical connections exhibit greater resistance to bending, fatigue, and torque loss compared to traditional designs. This translates clinically into a significant reduction in mechanical complications — screw loosening and component fractures decrease substantially (Merz et al., 2000; Velikov et al., 2019).
A particularly relevant finding concerns peri-implant bone preservation. Clinical evidence and meta-analyses indicate significantly lower marginal bone loss when conical connections are used — an effect that is even more pronounced in combination with platform switching.
Some dispute this claim. They say it reflects an outdated cultural bias. Fair enough, because:
“I disapprove of what you say, but I will defend to the death your right to say it.”
Evelyn Beatrice Hall
Regardless, this finding has significant clinical implications. Peri-implant bone preservation is one of the most important indicators of long-term implant success (Caricasulo et al., 2018).
The bone preservation characteristic of conical-connection implants is also operationally valuable. It allows implants to be placed relatively freely in infra- and subcrestally positions, compensating well for reduced mucosal thickness. This preserves the biologic width and prevents resorption — a principle central to our tailored regeneration approach.
Long-term system integrity has been confirmed by large retrospective studies analyzing thousands of implants. The data show very low implant and abutment fracture rates, particularly with wider taper angles, and high retrievability of seized abutments (Jin et al., 2022).
This is particularly important in daily practice, where maintainability is a critical factor for long-term success.
Current Challenges and Limitations
Conical connections have specific characteristics that may seem initially limiting compared to simpler designs.
The advantages far outweigh the drawbacks — but you need to know the system well to use it at its full potential.
Microgap
The presence of microgaps, albeit reduced compared to traditional designs, remains a clinical reality.
No system eliminates microgaps entirely.
These residual microgaps — typically 1 to 3 micrometers — still permit a minimal degree of bacterial infiltration. This can have significant implications in the peri-implant environment.
Microgap size is inversely proportional to manufacturing quality and production controls.
Wear and Deformation Under Load
A particularly interesting phenomenon emerging from the research concerns wear and deformation under cyclic loading.
Studies have shown that cyclic loading can increase microgap dimensions and induce wear phenomena — including fretting and adhesive wear — especially in the first 200,000 cycles. This raises important questions about long-term stability and requires careful monitoring over time (Yao et al., 2019; Rack et al., 2013).
This means the clinician must pay meticulous attention to occlusal contact adjustment, both centric and eccentric.
🎯 Critical Occlusal Control
Centric contact adjustment: Particular attention to uniform contact distribution in centric occlusion. Stress concentrations can induce premature wear of the taper coupling.
Eccentric movement control: Eliminate lateral and protrusive interferences that could generate lever forces damaging to the conical connection.
Occlusal follow-up: Schedule regular checks to monitor occlusal changes and intervene promptly.
Sensitivity to Manufacturing Precision
Design sensitivity is another critical factor. Conical connection performance depends heavily on manufacturing precision, cone angle, and coupling quality.
The more precise the component dimensions, the smaller the microgap. Narrower taper angles can increase the risk of deformation or fracture — something we observe frequently with certain manufacturers. This sensitivity demands high production standards and rigorous quality control (Gantier-Takano et al., 2025; Körtvélyessy et al., 2023).
The Complexity of Retrieval
Retrieval deserves particular attention. Tighter connections, especially those with smaller angles, can make abutment removal difficult when maintenance is required.
This phenomenon — while in a sense confirming the effectiveness of the retention system — can complicate revision or maintenance procedures.
Research has shown that cone angle significantly influences both stability and retrievability. Wider angles tend to facilitate removal; narrower angles offer superior retention but complicate maintenance. This balance represents one of the main challenges in optimal system design. The choice must always weigh the risk-benefit ratio for each individual clinical case.
Clinical Considerations for Daily Practice
Clinical application of conical connections requires a thorough understanding of their characteristics and limitations. Correct implementation is the key to success.
The versatility of these systems makes them particularly suited to complex clinical situations. They are ideal for immediate loading or demanding prosthetic rehabilitations, where functional micromovement must be minimized.
However, clinical success depends heavily on procedural precision and component quality. Not all conical systems are equal, and supplier selection becomes critical.
Selection of the appropriate taper angle must consider multiple factors. Choosing a system with a versatile angle that adequately balances retention and accessibility for maintenance is essential.
Reconstructive Complexity in Implant-Supported Bridges
When using an implant system with a true conical connection, compensating for divergence between cone insertion axes becomes necessary. This is critical when fabricating bridges on these prosthetic abutments.
With multiple implants restored by a bridge, even minor divergence cancels the excellent mechanical properties of conical connections. Alignment precision becomes fundamental.
In such cases, intermediate abutments are required to convert the conical connection into a flat-to-flat interface. This brings the connection to a juxta-mucosal position: these are multi-unit abutments, or MUAs.
In this way, the conical connection maintains excellent antibacterial sealing at depth. Simultaneously, the more external flat connection of the MUA allows bridge fabrication under optimal biomechanical conditions.
For Toronto-type prostheses — as with all bridges on conical connections — MUAs are indispensable.
Conclusions
Conical connections in dental implants undoubtedly represent a significant advance in implant technology. Technological evolution has delivered concrete, measurable clinical benefits.
The documented advantages in sealing, mechanical stability, and bone preservation are substantial and clinically relevant. These benefits translate into improved long-term implant prognosis.
It is important, however, to maintain a balanced perspective, acknowledging that these solutions are not free of limitations. Deep knowledge of the system is essential for clinical success.
The key is to know the (few) limitations so you can work around them and keep leveraging the advantages of the taper. Only then can we extract maximum benefit from this advanced technology, integrating it into a clinical approach that always prioritizes tailored regeneration for each individual patient.
Frequently Asked Questions
What is the main difference between conical and traditional connections? Conical connections (Morse taper) use a progressively tightening taper coupling that creates superior mechanical retention and significantly reduces microgaps compared to traditional flat designs — resulting in better sealing and mechanical stability.
Are microgaps completely eliminated with conical connections? No. Microgaps are drastically reduced, not eliminated. Residual microgaps of 1–3 micrometers remain, but this is still a significant improvement over traditional designs.
How much does the cone angle affect performance? Substantially. Wider angles ease abutment removal but reduce retention. Narrower angles offer superior retention but complicate maintenance and increase deformation risk.
Are conical connections harder to remove for maintenance? Yes — their greater stability can make abutment removal more complex. Studies show high retrievability, however, especially at angles that are not excessively narrow.
What are the main documented clinical benefits? Significant microgap reduction, greater mechanical stability, better peri-implant bone preservation, reduced peri-implantitis risk, and fewer mechanical complications such as screw loosening.
Are there specific contraindications for conical connections? No absolute contraindications. Success depends on manufacturing precision and the clinician’s knowledge of the system.
How do they perform under cyclic loading over time? Generally well — but microgap enlargement and wear can occur in the first 200,000 cycles before the system stabilizes.
Are they suitable for immediate loading? Yes. Their greater stability and reduced micromovement make them particularly indicated for immediate loading. Multiple-element loading requires MUAs.
FAQ
- What is the main difference between conical and traditional connections?
- Conical connections (Morse taper) use a progressively tightening taper coupling, creating superior mechanical retention and significantly reducing microgaps compared to traditional flat connections. This translates into better sealing and mechanical stability.
- Are microgaps completely eliminated with conical connections?
- No, microgaps are not completely eliminated but are drastically reduced. Conical connections typically retain microgaps of 1–3 micrometers, which still represents a significant improvement over traditional designs.
- How much does the cone angle affect performance?
- The cone angle is a critical factor. Wider angles facilitate abutment removal but may offer lower retention, while narrower angles provide superior retention but can complicate maintenance procedures and increase the risk of deformation.
- Are conical connections harder to remove for maintenance?
- Yes, the greater stability of conical connections can make abutment removal more complex when needed. However, studies show high abutment retrievability, especially with not excessively narrow taper angles.
- What are the main documented clinical benefits?
- Key benefits include a significant reduction in microgaps, greater mechanical stability, better preservation of peri-implant bone, reduced risk of peri-implantitis, and fewer mechanical complications such as screw loosening.
- Are there specific contraindications for conical connections?
- There are no absolute contraindications, but success depends on manufacturing precision and the clinician's familiarity with the system.
- How do they perform under cyclic loading over time?
- Studies show that conical connections maintain good performance under cyclic loading, although microgap increase and wear phenomena may occur in the first 200,000 cycles. After that, the system tends to stabilize.
- Are they suitable for immediate loading?
- Yes, conical connections are particularly indicated for immediate loading thanks to their greater stability and reduced micromovement — critical factors in these complex clinical situations. When loading multiple elements, MUAs are required.
Looking for a specialist?
Implantologia a Frosinone →Impianti dentali, carico immediato e rigenerazione ossea
Need a professional opinion?
Book an appointment at Dr. Bruschi's practice in Frosinone. First visit includes full diagnosis and personalised treatment plan.
Stai valutando un impianto dentale?
Ho scritto una guida in 8 capitoli che spiega tutto quello che un paziente dovrebbe sapere prima di sedersi in poltrona. Niente marketing — solo fatti, casi studio e una checklist per fare le domande giuste.
Scarica la guidaStay Updated
New articles on periodontology, implantology and oral surgery — delivered to your inbox.
Comments
Loading comments...
Leave a comment